Groundhog Day is an observance perfectly suited to this pandemic. We have traveled this way, seen this movie before. Will it ever end? Now that Punxsutawney Phil (accepting speaking gigs at groundhog.org) has seen his shadow, does that mean six more weeks of Omicron?
U.S. News & World Report noted recently that “Despite increasing immunity from Omicron infections and vaccines, experts say the transition from pandemic to endemic is still a ways away.” Well, how far is “a ways”? To paraphrase the Ad Council’s COVID-19 vaccination campaign, unveiled a year ago: It’s Up to Us.
On Groundhog Day a year ago, the U.S. passed the mark of 26 million COVID-19 cases. Today we’re over 75 million.
On the positive side: Cases and hospitalizations are trending down. Omicron is, on the whole, less severe than its predecessors.
However, we’re still averaging more than 2,200 deaths a day. Community transmission remains high in 99.75% of U.S. counties.
A year ago, we were just seven weeks into the vaccination campaign. We’ve come a long way, or ways, since then. Here’s where we stand today. May we not see a shadow.
• 250 million people have received at least one COVID-19 shot. A year ago it was 31 million.
• 75% of the country’s population and 80% of the vaccine-eligible (age 5 and up) have received at least one shot.
• Nearly 212 million are fully vaccinated (boosters not included). A year ago, that number was 8.5 million.
• 64% of the total population is fully vaccinated, 68% of everyone 5 and older.
• 88 million folks have had a booster or additional dose, including 45% of fully vaccinated adults. Another 85 million are booster-eligible.
Children tell a different story. Among kids ages 5 to 11, 20% are fully vaccinated, ranging from 7% to 8% in Alabama, Louisiana and Mississippi to 41% in Massachusetts and Rhode Island, 42% in Puerto Rico and 52% in Vermont. Mississippi last week recorded its 10th pediatric death of the pandemic. Among adolescents ages 12 to 17, 55% are fully vaccinated.
Pfizer and BioNTech are now asking the Food and Drug Administration to authorize use of their vaccine for kids 6 months up to 5 years of age
The Centers for Disease Control and Prevention continues to say that people who have received boosters are “up to date” on their vaccinations, while people who have had everything but a booster are “fully vaccinated.” Got it?
Whether your own COVID-19 prognosticating groundhog sees its shadow is very much a function of the weather where you live. Figuratively speaking, you may be just coming out of a coronavirus nor’easter—or still in its wicked path.
Here’s this week’s countdown.
10. The diagnosis: chronic COVID fatigue syndrome
“Fatigue and frustration dominate the public’s mood” is the takeaway from the latest Kaiser Family Foundation COVID-19 Vaccine Monitor, and these attitudes are shared by more than 70% of Democrats, Independents and Republicans. The foundation has been tracking “the dynamic nature of public opinion as vaccine development and distribution unfold” and has issued nearly 40 reports since December 2020.
Another attitude crossing party lines, KFF notes, is the belief—again, shared by more than 70%—that most Americans will eventually get COVID-19. Roughly 1 in 7 (14%) insist they will “definitely not” be vaccinated, a figure holding steady since December 2020. The number of “definitely nots” is even higher (25% or more) among rural residents, white evangelical Christians and Republicans.
Among people eligible for a booster, 39% want it as soon as possible. But 19% say they will definitely not get one, 16% prefer to wait and see and 22% will roll up their sleeves again only if required to do so.
34% consider “breakthrough” infections among the vaccinated a sign that the vaccines are not working. On the other hand, 62% assert that vaccines are in fact working because most people with breakthroughs do not need hospital care.
9. Fatigue is one thing, incivility quite another
The signs say “Aggressive or Disruptive Behavior Will Not be Tolerated.” It’s a sad commentary that they are posted on hospital walls throughout Hackensack Meridian Health, New Jersey’s largest health network. The signs caution against abusive or foul language, verbal and physical threats and assault.
“Our health care heroes are selfless and deserve our unwavering gratitude, respect and courtesy,” writes Hackensack Meridian CEO Robert Garrett in an op-ed for the USA Today Network. “They will be there in our darkest hour. We will get through this together with mutual respect and compassion.”
8. Mental health is the parallel pandemic
The pandemic has taken its toll on worker well-being, Mahalia Mayne reports in People Management. Of 2,000 employees surveyed in the U.K., 67% are feeling moderate to high levels of stress, more than half are fatigued, 28% have seen productivity suffer and 8% have contemplated self-harm.
Mental Health First Aid, a project of the National Council for Mental Wellbeing, offers guidance on how to survive another winter of COVID by prioritizing mental wellness. The organization, which believes that mental health first aid should be as fundamental as CPR, offers a number of resources to help build resiliency. Meanwhile, Education Secretary Miguel Cardona says that “our schools must offer increased access to mental health support for students.”
7. Spotify on, Spotify off
Legendary rocker Neil Young demanded that his music be taken off the streaming service Spotify because of vaccine misinformation spouted (spoutified?) on the platform by podcaster Joe Rogan. Spotify opted to roll with Rogan, whose podcasts draw an audience of 11 million. Ka-ching.
Now Campaign’s Imogen Watson says Apple Music is courting Spotify customers by making Young’s entire catalogue available. Joni Mitchell and other artists are joining Young and taking their talents elsewhere.
Just three weeks ago, a group of more than 270 doctors, nurses, professors and science communicators sent an open letter to Spotify, saying the platform is damaging public trust in scientific research. They called for “a clear and public policy to moderate misinformation.”
In response, Spotify said it will add a content advisory to any podcast discussing COVID-19, directing listeners to a hub listing trusted sources of information.
Rogan apologized for stirring controversy and promised to incorporate additional viewpoints into his podcasts. Both sides now?

6. The FDA shuffles the medicine cabinet
The Food and Drug Administration is taking steps to help keep COVID-19 patients out of the hospital. The antiviral branded as Veklury (remdesivir), previously limited to in-hospital use, is now available for non-hospitalized patients who have mild-to-moderate COVID-19 and are at risk for severe disease. Treatment is a three-day IV infusion. Brian Park has details in MPR.
Also available for the same clinical purpose—if you can find them—are two pills, molnupiravir and Paxlovid, which received FDA green lights in December.
In the meantime, the FDA has restricted the use of two monoclonal antibody combinations because they are “highly unlikely” to be effective against Omicron. The two are bamlanivimab/etesevimab and casirivimab/imdevimab.
That leaves sotrovimab as the one monoclonal antibody still in the Omicron dispensary.
Once more, with feeling: The FDA emphasizes that none of these treatments is a substitute for vaccination and boosting.
5. The movable mandate mentality
Yes, the Supreme Court put the kibosh on a nationwide plan to require COVID-19 vaccination or weekly testing at businesses with 100 or more employees. But no, mandates are not dead. More than 40% of private employers surveyed by Gartner are already requiring vaccination, Diane Eastabrook reports in McKnight’s Home Care, and more plan to do so. Also in McKnight’s Home Care, Liza Berger notes that 61% of adults said they would prefer to work for a company that mandates COVID-19 vaccination.
Meanwhile, the federal mandate for healthcare workers in hospitals, nursing homes and other Medicare-/Medicaid-funded facilities is moving forward, James M. Berklan notes in McKnight’s Long-Term Care News. It gets confusing, as the mandate will require employees in about half the states to be fully vaccinated by February 28 and in the other half by March 15. Oh yes—in Texas it’s March 21. That’s just the way the coronavirus cookie crumbles after all the action in court.
When it comes to enforcement, the Centers for Medicare and Medicaid Services won’t immediately pursue facilities that have achieved 80% vaccination of staff and have a plan to reach 100% within 60 days. Meanwhile, Berger reports, “Home care providers remain concerned that staff from organizations that must adhere to vaccine mandates will flock to those that are not bound by rigid vaccination rules.”
4. This week’s newsletter is brought to you by the number 4
Researchers have identified four possible factors for developing “long COVID”: pre-existing type 2 diabetes, blood levels of SARS-CoV-2 RNA, blood levels of Epstein-Barr virus DNA and specific autoantibodies.
Investigators from the Institute for Systems Biology published their findings in the journal Cell and said that long COVID occurs after mild as well as severe cases of COVID-19.
Immunocompromised people, who have difficulty generating a robust immune response to COVID-19 vaccine, are eligible for a fourth dose. But some have been turned away by pharmacies, Kaiser Health News reports. The CDC has reached out to pharmacies to clarify matters.
Novavax is seeking emergency authorization for its protein-based COVID-19 vaccine. It would become the fourth vaccine available in the U.S. and has already received nods of approval from the European Union and World Health Organization.
The FDA granted full approval Monday to Moderna’s COVID-19 vaccine, hereafter known as Spikevax, for adults. Full FDA approval for the Pfizer/BioNTech vaccine (does the name Comirnaty ring a bell?) came last August.

3. Say what you know and know what you say
The Government Accountability Office, a federal watchdog agency, has added the Department of Health and Human Services’ leadership of public health emergencies to its “high-risk list.”
The GAO says that “for over a decade, we have found issues with how HHS’s leadership prepares for and responds to emergencies, including COVID-19, other infections and extreme weather events, such as hurricanes.” Among five deficiencies cited was lack of clear and consistent communication to key partners and the public.”
CommCore Consulting Group offers some tips on “Crisis Communicating When the Facts Keep Changing”: Communicate often and provide the facts as you have them (caveat: know when it’s best to monitor and not respond). Sing from the same hymnbook (leaders should be on the same page whether communicating internally or externally). Share what you know (and if asked to speculate, don’t). Acknowledge that information will change as the situation changes. Avoid jargon. Provide a plan forward. Offer a measure of hope by explaining how the post-crisis situation will be better.
2. Seek education and ye shall find
Quite apart from HHS and CDC, COVID-19 educators are in plentiful supply and exerting their influence with less fanfare and not as much flak.
The Vaccine Education Center at Children’s Hospital of Philadelphia produces a regularly updated library of videos and infographics to educate families about COVID-19 vaccines. A new infographic looks at the risk of myocarditis—following vaccination and following COVID-19 infection—in young males ages 16 to 29. In a video, a pediatric cardiologist talks about myocarditis.
The Public Health Communications Collaborative has been issuing updates to communicators throughout the pandemic, offering helpful Q&As and talking points as the science has evolved. One of the latest is “Building Bridges: A practical communications tool for acknowledging tough questions and building trust.”
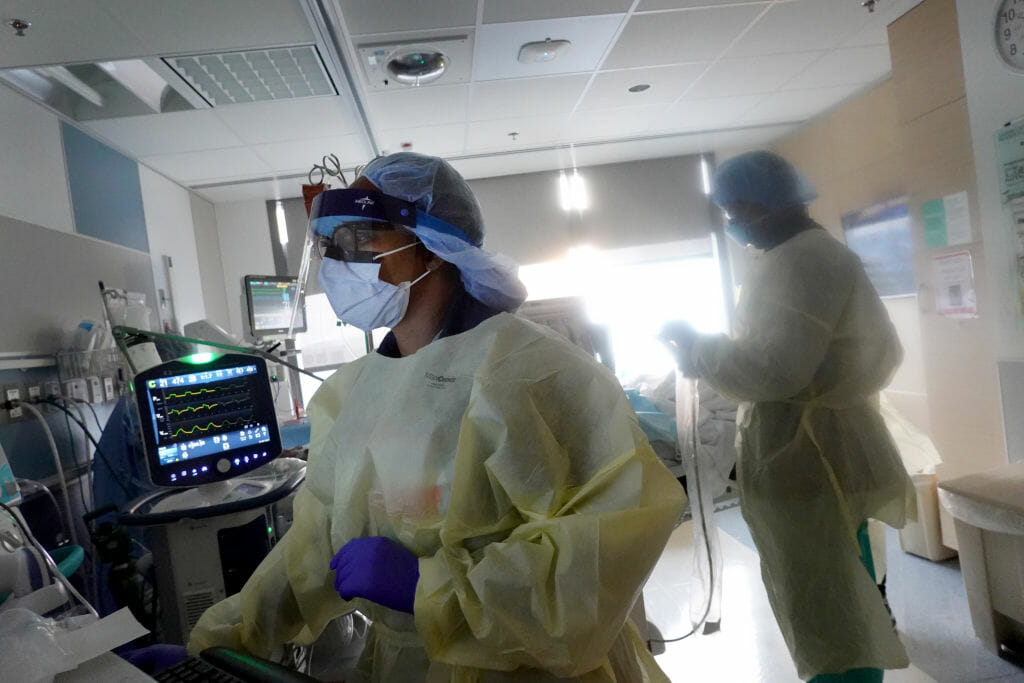
1. “Milder doesn’t mean mild”
While the sheer numbers of Omicron cases are overwhelming, the variant does appear to be causing less severe disease. The CDC reports a lower rate of infections that lead to emergency department visits, hospitalizations and deaths in the time of Omicron (December 19, 2021 to January 15, 2022) versus the time of Delta (July 15 to October 31, 2021) and the winter of 2020-2021. Hospitalizations are less severe as well: shorter stays, fewer ICU admissions and not as much use of invasive mechanical ventilation.
The CDC attributed the drop in disease severity to several factors, notably the increase in vaccination and boosters but also the protection afforded by prior infection and the presence of a less virulent variant. But CDC Director Dr. Rochelle Walensky cautioned, “Milder doesn’t mean mild.”
Some of us are old enough to remember that cigarettes were once widely advertised as “mild.” One ad featuring celebrities such as Marlene Dietrich and Rex Harrison declared, “Scientific tests prove Lucky Strike milder than any other principal brand.”
Science evolves. Today the FDA forbids tobacco companies from advertising products as “mild” or “light” unless they have obtained a Modified Risk Tobacco Product order. Yup, there is such a thing.
Parting shot
Here’s a headline from a year ago: “With demand far exceeding supply, it matters that people are jumping the vaccine line.” Today, with no lines to speak of and walk-ins welcome, the vaccine effort could use a shot in the arm.
Healthcare workers have an opportunity to educate, but they are not of one mind on the matter. An infographic in MM+M shares data from a recent study in the American Journal of Infection Control among nearly 2,000 healthcare workers, 15% of them unvaccinated. Most surprising: Only 73% of the unvaccinated say they believe in immunizations.
…and some songs
Better Times Will Come, Janis Ian
If I Could Turn Back Time, Cher
Good to see you. Again. Be well, stay well, enjoy your life, embrace your life. See you back here next week.








