Throughout the industry’s history, drugs and medical devices have — sometimes quite literally — been agents of significant change. Here are five products whose impacts resonate through time, and the stories behind them.
1962 | THALIDOMIDE
Regulators get assertive

 Assertive regulators — and multiple layers of regulation — are a fact of life for any modern-day copywriter or creative in healthcare advertising. But back in the 1960s, they were novelties. Thalidomide is the reason for that positive change.
Assertive regulators — and multiple layers of regulation — are a fact of life for any modern-day copywriter or creative in healthcare advertising. But back in the 1960s, they were novelties. Thalidomide is the reason for that positive change.
By the early 1960s, lingering problems beclouded the regulatory system for drugs. For one, said FDA historian John Swann in a 2012 podcast, products made it to market without being proved effective.
In 1959, Sen. Estes Kefauver (D-TN) began a series of hearings that, at the time, concerned price increases. But as they unfolded, other issues came to light, most notably the fact that many products that made it to market simply didn’t work as advertised.
Kefauver expanded his scope in 1961 to include the problem of ineffective drugs, introducing a bill to give the FDA enhanced control over investigations (and greater say over Rx advertising, after subpoenas to medical ad agencies demanded they defend their work). It drew substantial opposition in Congress.
Read more about the industry’s milestone moments in MM&M‘s 50th Anniversary issue.
Meanwhile, in September 1960 the FDA received an application from Cincinnati-based Richardson-Merrell for a sedative known as thalidomide, which the firm wanted to market under the brand name Kevadon. Thalidomide was already being sold in more than 40 countries to prevent morning sickness.
The application hit the desk of first-year FDA medical reviewer Dr. Frances Oldham Kelsey, who felt the company needed to submit chronic toxicity data to establish safety. Her refusal to approve the drug prompted a howl of protest from the company, which appealed to Kelsey’s superiors. But Kelsey, who had started her job at the agency a mere month prior to the application’s arrival, was unbowed.
Coincidentally, clusters of a severe birth defect known as phocomelia were showing up. Phocomelia is characterized by absent intrauterine long-bone formation, which resulted in babies’ hands emanating directly from shoulders or feet arising from hips. No one could account for its cause until late 1961, when a German physician and an Australian physician independently linked it to thalidomide.
The drug was immediately yanked from the market. Even with this global tragedy unfolding, the FDA application remained open until March 1962, according to Swann.
See also: 7 ways Viagra changed the ways drugs are marketed
Meanwhile, the bill that Kefauver had introduced in 1961 was struggling for support. Kefauver decided to leak the inside story about the thalidomide application to The Washington Post, which published a front-page article on America’s near tragedy and Kelsey’s lead role in preventing it.
Opposition to Kefauver’s bill quickly melted away. The 1962 Kefauver-Harris Amendments completely changed the face of drug regulation and gave the FDA a stricter hand with marketing.
Until that time, companies, said Swann, had been “taking considerable liberties when it came to advertising their products.” The new law reassigned control over prescription drug advertising from the FTC to the FDA, which would henceforth require all ads to include a “fair balance” presentation — effectiveness versus precautionary information — and a brief summary of the package insert.
And what of thalidomide? The drug that caused 8,000 to 10,000 birth defects worldwide and an untold number of stillbirths is now approved in the U.S. as a cancer treatment, under very strict regulation.
1976 | NAPROSYN
The birth of the medical brand persona
Emotion remains the spark with which audiences most identify, in pharma and medical device advertising alike. On the patient side, emotion traces its roots to Medicus’ 1980s ad for non-sedating antihistamine Seldane, one of the first to exploit the DTC channel before the rules were liberalized in 1997.
But one brand had forged an emotional persona long earlier: Syntex’s Rx analgesic Naprosyn. And it did so entirely on the basis of what used to be called “ethical” promotion — no consumer media or TV.
Its promotion debuted by early 1976, months before fellow NSAIDs Nalfon and Tolectin (although Motrin had come out a couple of years earlier), because its first set of ads featured only the package insert and risk disclosure, recalls Lester Barnett.
See also: 30 years later, DTC’s complicated past still hasn’t deterred marketers
In fact, restlessness would become a sort of calling card for Naprosyn, as it not only vied for a place in medicine chests but also ushered in the era of medical brand persona.
At the time, Barnett was the executive art director at San Francisco agency Barnum Communications, which held the account for Naprosyn. He attests to being “in the room” for a sort of anti-campaign moment: “I fought for ‘we are not doing a campaign, but creating a unique feeling proposition, building a brand personality.’”
Naprosyn — Bay Area pharma firm Syntex’s version of naproxen sodium — was the drug with which Barnett made his stand, and it became known as “the perpetual teenager.”
“That personality went beyond the campaign to become the very essence of the brand for its entire life span,” explained Barnett in a subsequent email. “All campaigns were weighed against the established ‘brand personality.’”
His efforts were preceded — and perhaps facilitated — by another important change agent: Herb Lubalin, who moved the pharma advertising world from the dominant Swiss style of the ’50s, with little brand differentiation, to campaign individualization via a broad range of typographic and design stylings.
See also: Merck’s creative archive tells an industry story
“Medical advertising could look and sound like advertising. It didn’t need to look like medicine anymore,” says Barnett.
After establishing its hyperactive persona, Naprosyn continually pushed the envelope with new dosages and forms — anything to make news — while competitors clung to reminder advertising.
It paved the way for many future brands to make individual names for themselves. Still, Naprosyn remains somewhat of an anomaly by current standards.
“Today’s business is an introduction business,” says Barnett, who is considered the godfather of branding. “No one supports the brand anymore. Naprosyn kept the perpetual teenager going.”
1987 | AZT
Patient power and the arms race on drugs
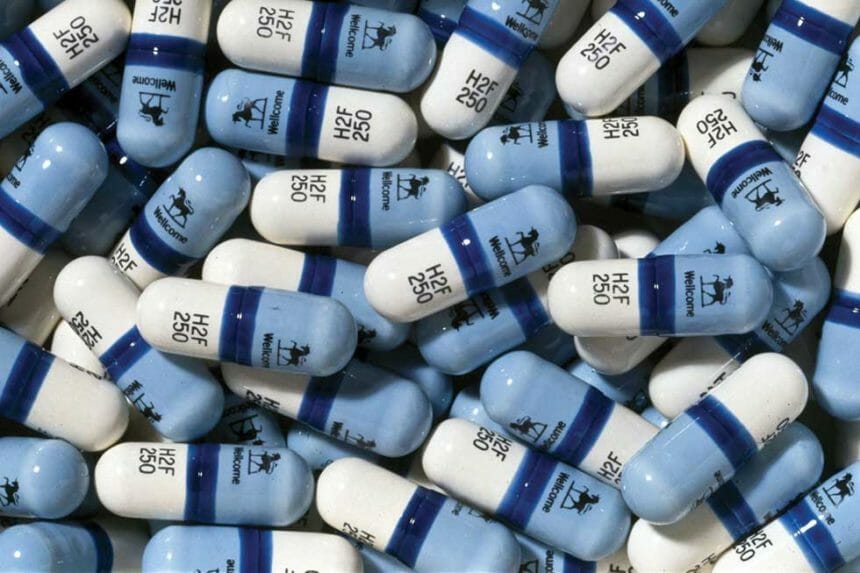
 Many of the talking points in today’s drug-pricing debate echo those when AZT reached the market. Photo credit: SSPL/Getty Images
Many of the talking points in today’s drug-pricing debate echo those when AZT reached the market. Photo credit: SSPL/Getty Images
Cost concerns for prescription drugs loom large, and medication remains priced beyond the reach of the sickest patients. Sound familiar? It was the national discourse in 1987.
That was the year AZT entered the pharmacopeia as the first treatment shown to lengthen the lives of patients with AIDS. As the only approved drug for the AIDS virus, AZT could fetch a premium price, a fact not lost on marketer Burroughs Wellcome (forerunner to GlaxoSmithKline).
“[AZT’s] original price was $10,000 a year. It started the arms race on drugs,” notes Michael Weinstein, the longtime HIV/AIDS activist who set up the AIDS Healthcare Foundation that same year.
Its price also sparked a new brand of activism, later called “vigilante consumerism” by one consultancy. In 1987, concerned individuals formed Act Up (AIDS Coalition to Unleash Power).
See also: Why the FDA’s view of patient communication evolved over time
Act Up staged a Wall Street demonstration to protest profiteering by pharma — especially Burroughs Wellcome — and the Reagan administration’s mishandling of the AIDS crisis. Shortly thereafter, the FDA said it would shorten its drug-approval process. A Wall Street sit-in by Act Up two years later led Wellcome to lower AZT’s price by 20%.
But it didn’t end well, because many people who started on AZT in ’87 died. Data from the National Center for Health Statistics show deaths in the U.S. due to AIDS climbed from about 13,000 in 1987 to just over 41,000 a year in 1995.
It wasn’t until 1995, the year following approval of Roche’s saquinavir, that the death rate began to fall. Prior to AZT, the sentiment was “do everything possible to get a treatment as soon as possible,” says Weinstein. Patients were taking to the streets demanding fast-track approval for promising therapies and greater access to clinical trials.
“It was a relatively new thing to have a patient constituency that involved,” Weinstein observes, especially one like the subsection of people with AIDS, who were mainly successful middle-class people. “They weren’t a disenfranchised group.”
This patient power forced pharma companies to re-imagine themselves as part of the patient-support continuum. Some, including Boehringer Ingelheim, Merck, and Pfizer, responded with social-responsibility efforts aimed at making HIV treatments more accessible.
1994 | CARDIOLOGY STENTS
Medical devices beat pharma to the web

Today, nearly every FDA-approved medical device and drug brand has an internet presence. That wasn’t always the case, agency execs recall.
In 1994, the first commercial-facing healthcare website appeared, and it was for medical device firm Cordis, at the time an independent maker of cardiology and endovascular products like bare-metal stents.
That device firms would be quicker than drug companies to use the internet makes sense, says Linda Holliday, who cofounded the agency that did the seminal web work for many device and pharma clients, Philadelphia-based Medical Broadcasting Co.
See also: The provider gift ban: The day the tchotchkes died
At the time, “the internet wasn’t seen as a commercial thing. It was a scientific thing, so researchers in those high-tech businesses — devices more so than drugs — understood it first,” Holliday points out.
A 1990s snapshot of Cordis.com (taken after the firm became part of Johnson & Johnson) shows its mission statement, main business lines, and little else. Companies eschewed adding product information.
“Corporations never talked to customers as corporations — their business lines or products did,” Holliday explains. “The audience for the corporate people was investors or employees. So pharma companies saw themselves through that lens and websites became digital versions of their corporate HQ.”
It was hard for pharma and device companies to even contemplate putting product information on their sites. Take J&J: “Moms in Iowa didn’t realize that when they bought baby powder, it was from the same company that made birth control, and this was scary and difficult to handle,” Holliday recalls.
According to her, MBC went on to do thousands of web properties for the likes of J&J, Merck, Pfizer, and others. As for Cordis, J&J picked it up in 1996 and then it changed hands again, last October. Its site is now merged into that of Cardinal Health’s.
2012 | ZALTRAP
Moneyball comes to healthcare

Patients compelled Burroughs Wellcome to lower the price of AIDS drug AZT in the 1980s. A couple of decades later, a group of physicians refusing to prescribe colon-cancer drug Zaltrap played agitator.
Dr. Leonard Saltz, head of GI oncology at Memorial Sloan-Kettering Cancer Center and head of its formulary committee, put it well at last May’s MM&M Transforming Healthcare Conference.
“Zaltrap was an interesting situation,” he recalled, “because from my perspective as a clinician — from our perspective as an institution — it offered absolutely zero benefit over a competitor at double the price. And therefore it’s half the value.”
That competitor was Genentech’s Avastin, and the rival biologic offered similar expected clinical outcomes for colorectal-cancer patients. Saltz was one of three MSKCC oncologists who explained the unflattering economic comparison in the opinion pages of The New York Times soon after Zaltrap’s August 2012 approval.
See also: Power to the payers: PBMs leave behind a trail of tiers
A few months later, Sanofi effectively halved the price of the drug, whose initial cost was $11,000 a month. It was a “watershed moment,” an insurance executive told the Times, both in terms of the size of an oncology drug’s price cut and of oncologists saying “enough is enough.”
Since then, the pressure on companies to meet provider and payer demands for such evidence has only increased, driven by Gilead’s decision in 2013 to price Sovaldi at $1,000 a pill.
Meanwhile, predatory pricing by the likes of Martin Shkreli (2015) and EpiPen’s manufacturer (2016), both on off-patent products, have again roused public ire. Some are calling drug pricing the healthcare issue of our time.
Have we just come full circle, back to the ’60s, when Sen. Kefauver trained a spotlight on drug price increases? Or to the charged atmosphere of the ’80s, when the AIDS community balked at AZT’s cost?
One thing seems certain, says Dr. Saltz — the “financial toxicity” of an agent is playing an increasing part in how patients value drugs.
“The idea that we can just hide this under the rug, which has been very comfortable for the past 50 years, is no longer tenable,” he says. “The sooner that those of us in the business of developing treatments understand this, the better off we will be.”
From the October 02, 2016 Issue of MM+M - Medical Marketing and Media