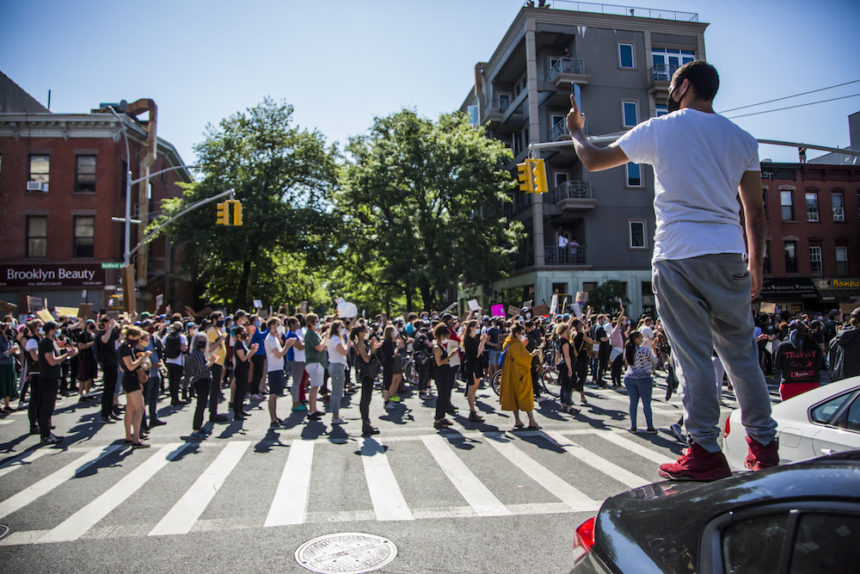The Black Lives Matter protests of the summer of 2020 were fueled by outrage over the deaths of George Floyd, Breonna Taylor and numerous other people at the hands of police officers. Yet, amid their calls for justice, accountability and more stringent police oversight, the protesters shone a light on a problem that has long festered in Black and other minority communities: A stunning and shameful degree of health inequity.
A Journal of the American Medical Association study published last year concluded that, between 1993 and 2017, there has been “a clear lack of progress” on remedying health inequity. The study called for “greater effort from public health policy makers, along with their partners in medicine and the sectors that contribute to the social determinants of health.”
As far as potential salves go, that’s not especially prescriptive. Which is why the greater health community is encouraged by the attention drawn by Black Lives Matter protesters and health-focused advocates to the scourge of health inequity.
“There seems to be a greater willingness for the general population to have more open conversations about the failings of a healthcare system that has historically deprived Black and brown communities of the same quality care given to white communities,” says Razorfish EVP, director of client services Ayanna Telfort.
However, she cautions this is just a start, rather than the breakthrough health leaders have long sought. “Unraveling the myriad threads that hold together a system designed to oppress one group of people in favor of another requires a tremendous amount of work, and those conversations can be contentious and difficult,” Telfort explains.
In a year like 2020, they don’t get any easier. “Historically, health equity and access was seen as a payer or government issue,” notes Publicis Health chief patient officer Susan Manber. “The tragic events of this summer have forced all of us to reckon with the ugly reality that racism pervades every aspect of our society.”
The status quo has proven stubbornly resistant to change, she adds. “This is a systemic issue requiring a systemic solution. That means adopting an approach that works across the continuum of care to address racism throughout the entirety of the system.”
So where does the medical-marketing community stand in its efforts to combat health inequity, as well as increase diversity and inclusivity in what has historically been a very white industry? “The [Black Lives Matter] movement has brought serious attention to the racial disparities in healthcare as well as the gross underrepresentation of BIPOC in marketing client teams and agencies — and thereby in the work itself,” says Heartbeat VP, human resources Michelle Edwards. “While uncovering these issues is an important step, there needs to be consistent, sustained action against systemic racism. And such action can begin by rebalancing the diversity of our professional community.”
Indeed, while few question its collective intentions, the marketing community doesn’t earn high marks for action. Asked whether marketers have accounted for disparities in health equity in their work, Razorfish VP, director of project management Funmi Olosunde says, “Short answer, no. Or at least not in any meaningful way, yet.”
Bellatrix Group founder and CEO Aurora Archer agrees. “Awareness is a critical first step, but it’s not enough,” she explains. “From R&D to clinical trials to commercialization to market penetration to the creation of wraparound services that truly serve a broader community, I wouldn’t point to any organization and say, ‘They’ve got it figured out.’”
For instance, within clinical trials Black and other minority audiences have long been underrepresented at best and ignored at worst. As a result, there’s a significant trust deficit among these groups that hasn’t been fully addressed. “Given the history of experimentation done on the Black community, how can there be trust?” asks Heartbeat VP, group account director Tiffany Marsh.
On the drug-marketing front, similar gaps exist. When people of color are featured in a campaign, usually it’s because, as Marsh puts it, “They are a large segment of their business.” So while Black people appear frequently in ads for diabetes medications, good luck spotting them in ads for, say, aesthetics or psoriasis.
“Representation in healthcare marketing is an issue, and that’s not even factoring in the gap in representation in medical books,” Olosunde says. Marsh agrees: “Such treatments that help resolve everyday annoyances or other life improvements are the territory of white people.”
One might argue that the disparities in access and treatment are worse now than they were a year ago. “The persistent murmurs about systemic health inequities for BIPOC people became full-blown shouts as it became clear that Black and brown people were being especially hard-hit by coronavirus,” Telfort notes.
To a person, experts say that any conversation about health inequity must start with an overt acknowledgement that racism is connected to healthcare — that, as Manber puts it, “Accessibility is about more than insurance. Where you live, transportation, quality of education, income stability and family/work responsibilities are all determinants that affect people’s access to and utilization of care.” One example from the COVID era: telemedicine, the successful utilization of which depends on internet access — which is more limited among Black people than among white people.
Most are optimistic that the influence of Black Lives Matter will continue to be felt in conversations about health inequity. But while companies have a range of assistance programs that, in theory, lower drug prices for the economically disadvantaged, these programs don’t begin to consider the factors that led to a disproportionate number of BIPOC individuals having a condition in the first place. Until the system begins to account for this, change will come in tiny increments, if at all.
“None of our overarching health issues will be solved if we don’t address these most fundamental issues of equity, care and access across our country,” Manber warns.
Telfort describes herself as optimistic, but suggests the time for talk is over and actual action is long overdue. “The global pandemic coupled with the civil unrest spurred by violence against Black people made such a powerful impact on our society that it’s difficult to walk away from this truth … No longer can we have innovation in isolated pockets of healthcare.”
From the November 01, 2020 Issue of MM+M - Medical Marketing and Media