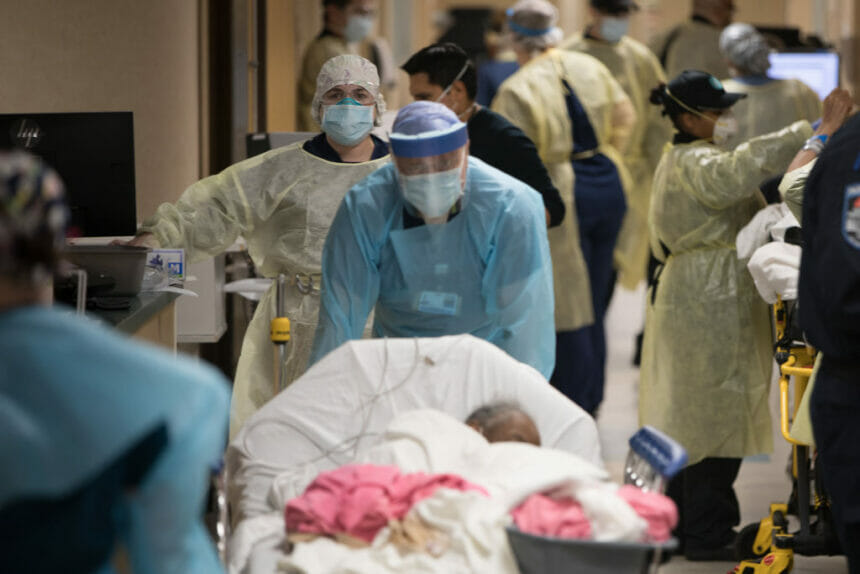
The COVID-19 public health emergency (PHE) officially ended in the U.S. on Thursday.
After more than three years since the PHE was first declared by then-Department of Health and Human Services (HHS) Secretary Alex Azar, the U.S. has exited the emergency phase of a pandemic that has infected millions and claimed the lives of more than 1.1 million citizens.
HHS Secretary Xavier Becerra released a statement acknowledging the end of the COVID-19 emergency phase but also emphasizing that the virus remains a “public health priority” for the agency.
“We have learned many lessons during the last two and a half years and have worked to strengthen our preparedness and response efforts by creating resiliency in the domestic supply chain, building capacity to ensure adequate stockpiles, and fostering innovation through projects like Project NextGen,” Becerra stated.
In early April, President Biden signed an end to the PHE but the last provisions lapsed on Thursday, including coverage for at-home COVID-19 and vaccine requirements for federal jobs.
The White House has said that it will focus on ensuring public health preparedness is prioritized going forward, calling for billions in funding as part of the 2024 budget proposal.
Similarly, Carlos del Rio MD, FIDSA, president of the Infectious Diseases Society of America, issued a statement imploring lawmakers that the time to “invest resources in preparedness is now.”
The effects of the changing status of the coronavirus outbreak in the U.S. has been notable over the past few weeks.
In Q1 earnings reports for several pharma companies, there were acknowledgements that the demand for COVID-19 vaccines, antivirals and tests are expected to decline in the coming months, hampering topline growth.
PhRMA CEO Stephen Ubl marked the occasion with an essay on LinkedIn, praising drugmakers for stepping up to develop vaccines and treatments that saved countless lives during the course of the pandemic.
“I want to note this milestone and thank the biopharmaceutical researchers, frontline workers, and other heroes who helped us reach this moment. Our work continues to help patients live longer and healthier lives,” he wrote.
Additionally, Dr. Rochelle Walensky, head of the Centers for Disease Control and Prevention, announced last week that she is resigning effective June 30.
Beyond the U.S., the World Health Organization also declared an end to the COVID-19 pandemic’s emergency status.
Where the healthcare industry goes from here remains an open question.
The virus is still lingering across the U.S., albeit it is not spreading or killing as many Americans as it did in years prior. That hasn’t stopped prominent healthcare organizations from issuing advisories featuring public health experts on what patients need to know going forward.
An expert at the Johns Hopkins Bloomberg School of Public Health questioned whether this was the right time to curtail certain pandemic-related provisions like easier access to Medicaid enrollment and supplying personal protective equipment to schools.
A professor at Emory University stressed that people should still stay up to date on their COVID-19 vaccinations and cautioned that the end of the PHE will likely have the most significant impact on uninsured patients.
A collection of researchers from RAND Corp. added that battling misinformation around COVID-19 is likely to be a challenge for healthcare organizations and public health officials going forward.